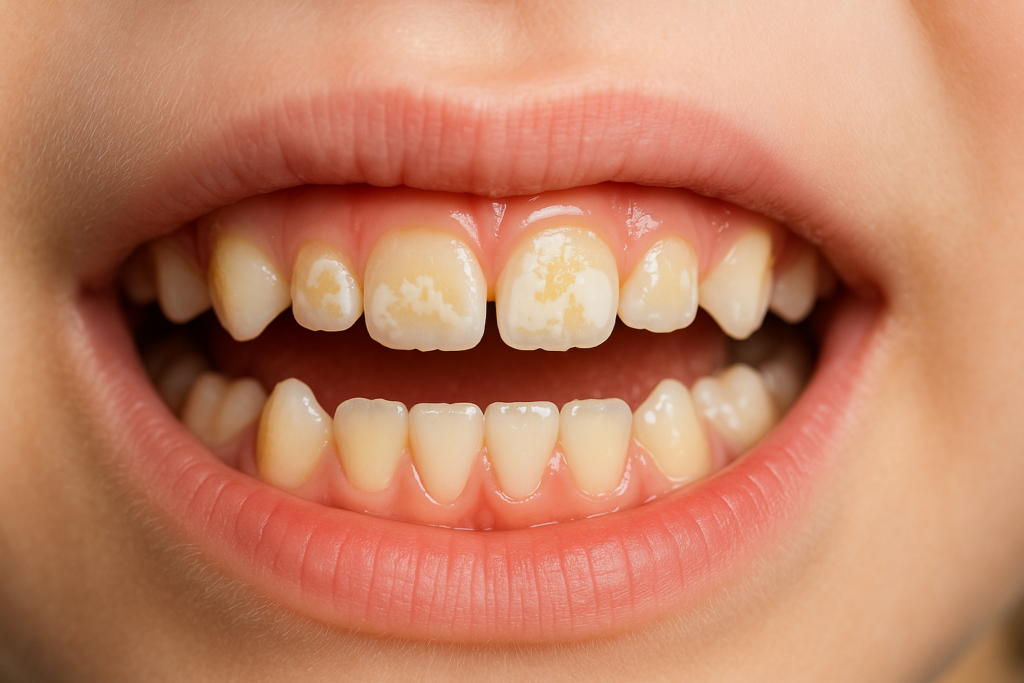
Parents often notice white, yellow, or brown “chalky” patches on their child’s teeth and wonder if it’s serious. If this sounds familiar, you’re not alone. Enamel hypomineralisation in kids can make teeth sensitive, prone to decay, and hard to clean. The good news: with the right plan, you can protect your child’s smile.
This guide explains what’s happening, why it occurs, how dentists treat it, and what you can do at home. We also share when to see a pediatric dentist at Pure White Medical Center and how our team in Mirdif, Dubai, supports young patients with gentle, evidence-based care.
Keep reading to feel informed and confident about your next steps.
What Enamel Hypomineralisation Means for Children’s Teeth
Enamel hypomineralisation is a qualitative enamel defect. The enamel forms, but it’s weaker and more porous than normal. That’s why teeth may look patchy (creamy-white, yellow, or brown) and feel sensitive to cold or brushing.
In contrast, enamel hypoplasia in kids is a quantitative defect—there is less enamel, often with pits or grooves. Clinically, both can coexist, but the distinction guides care.
Many children with hypomineralisation show it in first permanent molars and sometimes incisors—a pattern known as molar–incisor hypomineralisation (MIH). Affected teeth are at higher risk for breakdown, cavities, and pain, especially soon after eruption.
How Common Enamel Hypomineralisation Is in Children
Estimates vary by region and study methods, but large reviews suggest MIH affects roughly 13–16% of children worldwide. A 2021 systematic review found a pooled prevalence of 13.5%; newer analyses place MIH around 14–16%, with broader enamel hypomineralisation (EH) estimates sometimes higher.
Why does the range seem wide? Studies differ in how they diagnose and which ages they include. Still, the takeaway for parents is clear: enamel hypomineralisation is common, and your child is not alone.
Early Signs of Enamel Hypomineralisation Parents Can Spot
Look for well-defined patches on the biting surfaces or visible front areas of teeth. Creamy-white spots may appear mild; yellow-brown areas often signal softer enamel and a higher risk of chipping (called “post-eruptive breakdown”). Children may avoid cold drinks or struggle with brushing due to pain.
These are hallmark features of hypomineralisation teeth that kids often present with, and they justify an early pediatric dental visit.
Why Enamel Hypomineralisation Happens in Kids
There is no single proven cause. Research points to multifactorial influences during late pregnancy and early childhood (the period when enamel matures): early-life fevers or illness, low birth weight, environmental exposures, or certain early antibiotics have all been studied.
However, evidence is mixed, and no single factor explains most cases. Current guidelines emphasize individualized assessment and timely prevention, rather than chasing one cause.
Hypomineralisation in Baby Teeth and What It Means
Yes, hypomineralisation of baby teeth happens, particularly in second primary molars (sometimes called HSPM). It can predict a higher chance of MIH in the permanent molars later. Catching it in the primary (baby) teeth lets us start preventive care sooner and tailor follow-ups as the permanent molars erupt around ages 6–7.
How Enamel Hypomineralisation Is Diagnosed at Pure White Medical Center
A pediatric dentist can diagnose enamel hypomineralisation with a careful visual exam and gentle tests for sensitivity.
At Pure White Medical Center, our pediatric team creates a calm environment for kids, using age-appropriate explanations and behavior guidance so visits feel safe and positive. If needed, we coordinate care with other specialists. Learn more about our طب الأسنان للأطفال services and our specialists.
Treatment Options for Children with Enamel Hypomineralisation
Management depends on severity (mild color change vs. breakdown and pain), your child’s age, and cooperation level. The aim is to reduce sensitivity, prevent decay, and protect tooth structure—ideally before breakdown occurs.
Desensitization and Remineralization for Sensitive Teeth
For milder cases, dentists often use fluoride varnish and recommend home care with high-fluoride toothpaste (age-appropriate dosing) or calcium-phosphate creams (e.g., CPP-ACP) to strengthen enamel and ease sensitivity. Evidence suggests CPP-ACP can improve mineral density and surface hardness in MIH-affected enamel in the short term, though protocols and benefits vary among studies.
Randomized studies also explore hydroxyapatite vs. fluoride dentifrices for MIH, with promising in-situ data for remineralization; your dentist will choose what best suits your child and aligns with current guidelines.
Sealants and Minimally Invasive Restorations for Hypomineralised Teeth
On first permanent molars with intact (or minimally broken) enamel, fissure sealants or preventive resin restorations can block bacteria and reduce sensitivity.
Hypomineralised enamel can be tricky for bonding, so dentists may use glass-ionomer as an interim sealant and later switch to resin once the tooth stabilizes. Preventive sealants are part of our طب الأسنان الوقائي approach.
Restorations and Crowns for Severely Affected Teeth
When breakdown is moderate to severe, stainless steel crowns (for molars) protect the entire tooth, control sensitivity, and reduce the need for repeated drilling. For front teeth with color changes, options range from microabrasion and resin infiltration to composite bonding, balancing esthetics with enamel preservation. These choices follow international best-practice guidance for MIH.
Managing Pain and Anxiety in Children with Hypomineralisation
Local anesthesia can be less effective in MIH molars due to inflamed pulpal tissues. Pediatric dentists plan ahead with behavior guidance, supplemental anesthesia techniques, and, when appropriate, sedation options to keep kids comfortable. Our team emphasizes gentle, step-wise care tailored to your child’s needs.
When Extraction Is the Best Option for Hypomineralised Teeth
In a small subset of severe cases, planned extraction of badly affected first permanent molars—timed with an orthodontist—can lead to better long-term bite and alignment. The European Academy of Paediatric Dentistry supports considering this path when restorations are unlikely to succeed.
Home Care Tips for Children with Hypomineralisation
Daily habits can reduce sensitivity and decay risk. Brush twice daily with fluoride toothpaste (a smear for under 3; a pea-sized amount from 3–6; age-appropriate thereafter), and supervise brushing to ensure gentle technique on tender spots. Rinse with water after snacks if brushing isn’t possible. If cold hurts, try lukewarm water for rinsing. Keep regular checkups—early adjustments prevent bigger problems.
Smart Nutrition for Kids with Sensitive or Weak Enamel
Soft, mineral-poor enamel needs extra protection. Limit frequent sugary or acidic snacks and drinks (juices, sodas, gummy treats). Offer calcium-rich foods and water between meals. For kids with sensitivity, cool—not icy—foods are often better tolerated. Your dentist may recommend professionally applied fluoride at intervals based on risk.
Evidence from Studies on Enamel Hypomineralisation
- How widespread? Global estimates for MIH hover around the low- to mid-teens percentage of children; more recent meta-analyses place MIH around 14–16%, while enamel hypomineralisation more broadly may be higher.
- Do treatments help? Clinical trials suggest CPP-ACP and fluoride approaches can reduce sensitivity and support remineralization; other studies are assessing silver diamine fluoride (SDF) and CPP-ACP fluoride varnish combinations on MIH molars. Talk to your dentist about the latest protocols suited to your child.
How Pure White Medical Center Supports Children with Enamel Hypomineralisation
At Pure White Medical Center in Mirdif, Dubai, our pediatric team focuses on prevention, comfort, and durable results for children with enamel hypomineralisation. We start with a gentle exam, create a personalized plan (from desensitizing care to sealants or crowns), and track progress as new teeth erupt. Explore طب الأسنان للأطفال, طب الأسنان الوقائي, and our full list of services. To book directly, you can also use our appointment page.
Have questions or need an urgent check? Email Info@purewhitemedical.ae or call 050 251 0882. You can also contact us to find our hours and location.
Frequently Asked Questions
What is the difference between enamel hypomineralisation and enamel hypoplasia in kids?
Hypomineralisation is about weaker mineral content in enamel that formed to normal thickness, leading to chalky patches and sensitivity. Hypoplasia means less enamel was formed, often with pits or grooves. Both can increase decay risk, but treatments differ. A pediatric dentist can tell them apart and plan care that reduces pain and protects teeth.
Can hypomineralisation in baby teeth predict issues in permanent teeth?
Yes. When second primary molars show hypomineralisation, children may be more likely to develop MIH in first permanent molars later. This matters because early preventive steps, like fluoride varnish, sealants, and closer recall, can reduce breakdown and pain once permanent teeth erupt.
Are sealants reliable on hypomineralised teeth?
They can be, but technique matters. Hypomineralised enamel bonds differently. Dentists may place a glass-ionomer sealant first (it’s more forgiving in wet conditions) and later replace it with a resin sealant as the tooth stabilizes. The goal is to block bacteria in the grooves and reduce sensitivity.
When would a dentist suggest a stainless steel crown for my child?
If a molar has moderate to severe breakdown or persistent sensitivity, a stainless steel crown can protect the whole tooth and improve comfort. It often reduces the number of future visits compared with repeated fillings, which is important for anxious children. Your dentist will consider age, tooth eruption stage, and bite.
Is extraction ever the best option for MIH molars?
Sometimes. In very severe cases with poor prognosis, a timed extraction, planned with an orthodontist, can yield better long-term alignment. This decision follows careful assessment of tooth condition, root development, and overall bite. Families receive clear guidance before any step.